Antibody-drug conjugates have earned their reputation as one of the most exciting advances in oncology. The concept is compelling: engineer a molecule that delivers a cytotoxic payload precisely to tumor cells, minimizing the systemic damage that has long defined chemotherapy.
Yet for every ADC that reaches approval, many more stall in development – not because the science is flawed, but because the path from discovery to clinic is far more complex than initial promise suggests.
If you’re making decisions about ADC programs – where to invest, which candidates to advance, which partnerships to prioritize – understanding where development breaks down is as important as understanding the biology itself.
Here are the five challenges that most consistently slow ADC program progress, and what leading teams are doing to address them.
Read more: What Are Antibody-Drug Conjugates (ADCs)? Organoid Platforms for ADC Research
In This Article
Target Selection Remains Difficult in Heterogeneous Tumors
Every ADC starts with a target. The ideal: a surface antigen expressed uniformly and exclusively on cancer cells. The reality is rarely that clean.
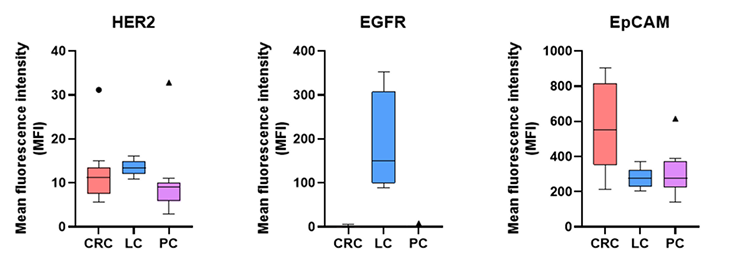
Even well-validated targets like HER2 and TROP2 show significant expression variability – across patients, across tumor subtypes, and even within the same tumor mass. A 2025 Nature Communications study that performed RNA sequencing across 909 samples from 30 metastatic breast cancer patients confirmed that target expression – including TROP2 and HER2 – is reduced in metastases compared to primary untreated tumors, and that heterogeneity is a meaningful variable across tissue sites.
This heterogeneity creates compounding problems for ADC efficacy. In tumor regions with low antigen expression, the ADC has fewer binding sites and reduced internalization – blunting drug delivery at the cellular level. In healthy tissue where the same target appears at low levels, unexpected on-target, off-tumor toxicity can emerge.
The downstream effect: a target that looks robust in early discovery may perform unpredictably when exposed to real tumor complexity. Tumor heterogeneity has been identified in ASCO educational reviews as a proposed mechanism of resistance to ADC, particularly for agents whose activity is strongly dependent on target antigen expression levels.
What this means for your program
Target validation strategies need to account for spatial and inter-patient antigen variability from the outset – not just average expression levels in a cell line panel. Programs that incorporate heterogeneity modeling early tend to reach better-informed go/no-go decisions.
ADC Toxicity and the Narrow Therapeutic Window
The promise of ADCs has always included an improved safety profile relative to conventional chemotherapy. That promise holds in principle. In practice, ADC toxicity continues to be one of the most common reasons programs are halted, dose-limited, or fail to advance.
The mechanisms are well-documented. On-target, off-tumor effects occur when healthy tissues express the same antigen being targeted. Premature payload release – driven by linker instability in circulation – leads to systemic drug exposure before the ADC reaches the tumor. Non-specific uptake by macrophages and other normal cells compounds the problem.
The clinical evidence is sobering. A 2025 analysis from ESMO Open of 163 patients across 19 ADC trials found that treatment-emergent adverse events occurred in 84% of patients, with grade 3–4 events in 29%. A separate Royal Marsden phase I cohort (2014–2024) reported toxicities including fatigue (48%), neuropathy (26%), ocular toxicity (26%), and pneumonitis (8%) – several of which were unexpected based on the payload mechanism alone.
Because ADC payloads are inherently potent – designed to kill cells at very low concentrations – even modest off-target exposure can translate into hematologic, hepatic, or pulmonary toxicity. The therapeutic window, while wider than traditional chemotherapy in many cases, remains narrow enough to define the ceiling on both dose escalation and efficacy.
What this means for your program
Toxicity risk cannot be managed at the clinical stage alone. Earlier, more sensitive preclinical models that capture off-tumor biology are increasingly necessary to predict and de-risk these outcomes before first-in-human trials.
ADC Linker Design and Payload Complexity
The linker connecting antibody to payload may be the most underestimated component in ADC design. It has one job – to keep the payload stable in circulation and release it inside the tumor – but executing that with precision is technically demanding and often unpredictable.
A linker that is too stable fails to release the payload at the tumor site, leaving the cytotoxic drug locked inside an intact conjugate. One that is too labile releases drug prematurely into circulation, reintroducing the systemic toxicity that ADCs are meant to avoid. Cleavable linkers offer flexibility but introduce stability risks; non-cleavable linkers improve stability but require full lysosomal degradation of the antibody for payload release – limiting the targets they can effectively reach.
Payload hydrophobicity adds further complexity. Many potent payloads – including auristatins and maytansinoids – are highly hydrophobic, which compromises pharmacokinetics and can cause ADC aggregation, faster clearance, and a narrower therapeutic index. Research has confirmed that ADCs with higher drug-to-antibody ratios (DAR) show faster systemic clearance, lower tolerability, and reduced in vivo efficacy compared to those with lower DAR – demonstrating that even small variations in conjugation chemistry can have large biological consequences.
The number of clinically validated payload classes also remains limited, which constrains the design space for next-generation ADC programs.
What this means for your program
ADC linker-payload optimization is not a linear process. Teams that invest early in understanding the relationship between chemistry, PK, and in vivo behavior – rather than treating these as separate workstreams – tend to make faster, better-informed decisions.
The Predictive Gap in ADC Preclinical Models
This is where many ADC programs quietly lose ground. The drug design may be sound. The target may be well-chosen. But if the model used to evaluate the candidate does not accurately reflect human tumor biology, the data it generates will be misleading – and the clinical attrition that follows is predictable.
Standard 2D cell cultures lack tumor architecture, stromal interactions, and the spatial heterogeneity of antigen expression that defines real tumor biology. Animal models, while useful for PK/PD bridging, frequently diverge from human pharmacokinetics and immune context in ways that matter specifically for ADCs.
ADC performance is a function of multiple dynamic processes: antigen binding, receptor internalization, intracellular trafficking, endosomal processing, payload release, and bystander activity. If the preclinical model does not replicate those processes with reasonable biological fidelity, then the efficacy and safety readouts it generates may simply not translate to patients.
Research published in Science Advances confirmed that the complexity of ADC design and the lack of robust predictive heuristics make it particularly difficult to determine whether a preclinical ADC candidate will succeed in the clinic. The gap between animal model response and human clinical outcome is not a minor calibration issue – it is a structural problem that contributes directly to high ADC attrition rates.
What this means for your program
The quality of your preclinical data is ultimately a function of model selection. As more physiologically relevant platforms become available – including 3D tumor models and patient-derived systems – there is a growing competitive advantage for teams that adopt them earlier in development.
Tumor Penetration and Intratumoral Drug Distribution
Even a well-designed ADC with a validated target and optimized linker-payload chemistry still needs to physically penetrate and distribute within solid tumors. This is harder than it sounds – and it is a challenge that is frequently underweighted in early ADC development.
Solid tumors are structurally hostile to drug delivery. Dense extracellular matrix, irregular and inefficient vasculature, and elevated interstitial pressure all limit how deeply and evenly a large molecule like an ADC can penetrate beyond the tumor margin. The result is heterogeneous intratumoral distribution -some regions receive therapeutic drug concentrations, while others do not.
This uneven exposure, layered on top of existing antigen heterogeneity, creates conditions favorable for resistance. Cancer cells in undertreated regions survive, continue to proliferate, and can repopulate the tumor – a dynamic that is increasingly recognized as a driver of ADC treatment failure in solid tumors.
A ScienceDirect review of ADC development challenges explicitly identified tumor delivery barriers as one of the most critical – and underappreciated – obstacles to realizing the full potential of ADCs in precision oncology.
What this means for your program
Delivery within the tumor – not just delivery to the tumor – is a meaningful variable in ADC efficacy. It deserves dedicated evaluation, not just an assumption of adequate penetration based on bulk tumor uptake data.
How Lambda Biologics Supports ADC Development Programs
At Lambda Biologics, we work with oncology teams navigating these challenges. Our organoid-based evaluation platforms are designed to provide more biologically relevant data on ADC efficacy and safety – across heterogeneous tumor populations and in three-dimensional tissue contexts that better reflect the clinical reality your program will eventually face.
Specific areas where our platforms are applied in ADC development include:
- Efficacy evaluation across patient-derived tumor models with variable antigen expression
- Early toxicity assessment in 3D systems that capture on-target, off-tumor biology
- Drug penetration and intratumoral distribution modeling in organoid architectures
- Translational data packages supporting IND-enabling studies and program decisions
Lambda Biologics’ Oncology Solutions: Patient-derived cancer organoid-based drug evaluation service
Gastric Cancer Organoid | Breast Cancer Organoid | Hepatocarcinoma Cancer Organoid | Pancreatic Cancer Organoid